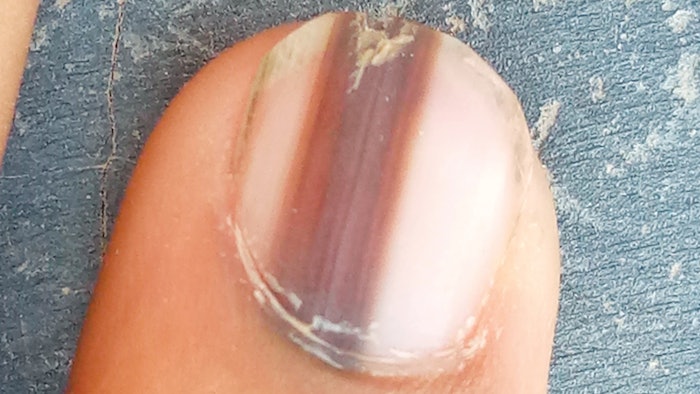
Subungual melanoma, a type of skin cancer under the nail, can go undetected because it typically appears in a toenail, which many people keep obscured with nail polish much of the time and just generally don’t spend a lot of time examining, says Austin, Texas, podiatrist Anne Sharkey. Ninety-two percent of subungual melanomas show up in the big toe or thumbnails but can affect any nail. They can look like black or brown streaks running from the cuticle to the nail tip. People often might dismiss melanoma as a bruise resulting from a stubbed toe or banged-up thumb. But unlike a bruise, it won’t go away as the nail grows.
“A trauma blood blister grows and moves, whereas with melanoma, it doesn’t move because the discoloration isn’t in the nail, it’s in the skin under the nail,” Sharkey says. “Trauma grows out, but melanoma wouldn’t change.”
Subungual melanoma is much more common among people of color, who often have streaks in their nails that are not cancerous, which makes detection more difficult.
“People of color are more likely to have multiple pigmented bands and more pigment in general, so it’s very challenging,” says Jerome R. Potozkin, M.D., a dermatologist in Danville, California.
No one expects nail techs to become experts at cancer diagnosis, but they can provide a life-saving link between clients and health care providers by familiarizing themselves with the disease, Potozkin says. Who’s at risk?
More than 1 million people in the United States have melanoma, and cases of it doubled between 1982 and 2011, according to the American Academy of Dermatology Association (AADA). The AADA also notes melanoma was expected to kill more than 7,000 people annually. But subungual melanoma is a pretty rare form of it, making up between .7 and 3.5% of malignant melanomas worldwide. Melanoma of the hands and feet only make up 2% to 3% of melanoma diagnoses in the U.S.
Only 2% of subungual melanoma cases occur in Caucasian people, whereas it’s the most common type of malignant melanoma among Black people, Asians and Hispanics. Subungual melanoma accounts for 75% of melanomas in African populations, 25% in Chinese populations and 10% in Japanese populations. Men are more susceptible—the ratio of cases affecting men outnumber cases in women 3:1. Like most cancers, it’s more common among older folks, with a median age of 65.
Causes of Subungual Melanoma
Unlike most melanomas, subungual melanoma doesn’t stem from sun exposure. Technically, it occurs when there’s increased melanin production and repeated injuries of the fingers or toe nails are considered a risk factor. Genetics likely also factor in, Potozkin says, but specific causes of subungual melanoma aren’t yet understood.
“Any cancer is the unregulated growth of cells,” Potozkin says. “Melanoma is the unregulated growth of melanocytes, the pigment-producing cell in the body. The scary thing with melanoma is that it has the tendency to metastasize and spread to other parts of the body. So, if diagnosis is delayed, it can be a life-threatening skin cancer.”
How It’s Diagnosed
Doctors look for patterns or characteristics of discolored nails, Sharkey says. They ask patients how long ago lines showed up on the nail, for example, or whether lines have changed or increased. Women who often wear really pointy, high-heel shoes put chronic pressure on some areas of the foot, which might cause bruising. To rule that out, Sharkey asks patients about shoes they typically wear. Skin cancer shows up primarily in one nail, Sharkey notes, so dark bands on multiple nails might not indicate cancer.
“Oftentimes in darker-complected patients, we notice one band changing and becoming bigger, wider and darker,” Potozkin says.
In addition, because it’s common in darker-skinned patients to see multiple bands on nails, it’s important to look for Hutchinson’s sign: pigmentation around the nail folds, or tissue that encloses the nail matrix at the nail root, he continues.
When evaluating a patient’s risk factors for subungual melanoma, doctors consider a set of guidelines referred to as “ABCDEF,” Potozkin says:
A. Asian and Black patients are at higher risk
B. Brown or black bands greater than 3 millimeters with irregular borders
C. Changes in size of the bands
D. Discoloration on the nails of the thumb, big toe or index finger
E. Extensions of discoloration into surrounding skin
F. Family history of melanoma
“If someone with a family history of melanoma sees a dark band on a nail, it’s very important to have it looked at, even if the patient is Caucasian,” Potozkin says.
If cause for concern, doctors will do a biopsy, which means taking a tiny tissue sample and examining it under a microscope.
“The prognosis depends on how thick it is under the microscope,” Potozkin says.
If the biopsy reveals melanoma, the only treatment option is surgery. Doctors typically will remove the nail and if they have to, they’ll remove the toe. But generally, surgical treatments are less aggressive today than in decades past.
This is why early detection of subungual melanoma is so important, Potozkin says. Diagnosing it before it’s too late saves fingers and toes from amputation and also stops the cancer from spreading to other parts of the body, which is called metastasization and is often deadly.
Education and Advising Clients
Despite efforts to educate the public about subungual melanoma in the last couple of decades, awareness of this type of cancer remains poor, noted the authors of a paper published in the Journal of the American Academy of Dermatology in 2018. This is why nail techs, who interact with people who might not see health care providers regularly, are a crucial piece of the detection puzzle, they wrote.
For the entire article, please check out Nailpro's May/June 2021 digital magazine.
![[VIDEO] How-To Rid Feet Of Calluses in 8 Steps](https://native-x.imgix.net/allured/664d0539682eac000179baef/Thumbnail_NativeX.jpg?crop=focalpoint&fit=crop&fp-x=0.5&fp-y=0.5&h=191&w=340&auto=format%2Ccompress&q=70)










