Unfortunately, years later, MRSA continues to be a concern in salons. In November 2009, Fox 10 News on the Gulf Coast reported that a salon client in Alabama was cut with an emery board several times during a routine manicure, leading to severe pain, swelling and redness. A doctor diagnosed her with staph in five of her fingers—luckily, before amputation was necessary. You can’t change the fact that this may happen in a salon, but you can prevent it from happening in yours by understanding what MRSA is and how to prevent it.
Understanding MRSA
Many nail techs have wondered what MRSA is and why it has become so newsworthy in the past few years. “MRSA is a common bacterium (staph) that causes skin infections that have become resilient to several antibiotics,” explains Vicki Malo, BScPod, CEDESCO, RMTA, president of the North American School of Podology in Toronto and member of the International Pedicure Association Advisory Board. “At one time, MRSA was found only in healthcare settings, such as hospitals and nursing homes, but now MRSA is being found in gyms, spas, health clubs, schools—anywhere there is direct skin contact.” These more recent infections, which usually occur in otherwise healthy people, are referred to as community-associated MRSA, or CA-MRSA.
In the United States in 2008, 18,000 people died from MRSA, says Malo. In other words, you and your clients are justifiably concerned; MRSA is easily spread and more common than ever. “The pathogen is now out in the community,” warns David Calfee, MD, associate professor of medicine, infectious diseases at Mount Sinai Medical Center in New York. “It’s spread through a person who is infected with or carrying the organism; this can mean skin-to-skin contact or indirect contact, such as touching something that has been contaminated.” Calfee recalls that a few years ago outbreaks were common on sports teams due to shared towels and, thanks to all of the communal equipment and surfaces in a salon’s intimate setting, no one was surprised when MRSA made its way to the beauty industry.
Indeed, MRSA exists everywhere in society. “Staph is a ubiquitous organism, one we will never eradicate completely,” says Aaron E. Glatt, MD, FACP, FIDSA, FSHEA, president and chief executive officer of New Island Hospital in Bethpage, New York, and spokesperson for the Infectious Diseases Society of America. “Skin is not sterile, and in the past 10 years, we have seen more frequency in the general population that is colonized with MRSA.” Infection most easily occurs after exposure to MRSA when there is a breach in skin, such as a cut, a nail infection or even a hangnail. But many people can have staph on their skin and not experience a problem; Glatt states that this is because being colonized with staph is different from being infected by it—people who are colonized have no signs or symptoms of infection.
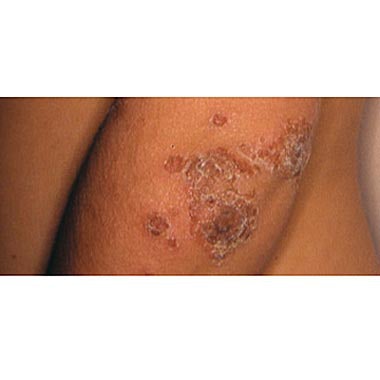
For those who are infected, the symptoms of MRSA are noticeable, but some clients may ignore them, misjudging them as mere cosmetic issues. “MRSA infections may appear as a reddened, swollen, tender area of skin called cellulitis; there may also be pustules or boils,” relates D’Anne Kleinsmith, MD, dermatologist in private practice in West Bloomfield, Michigan. Some treatments that may be successful, she explains, include doxycycline and tetracycline (antibiotics often used to treat acne), which are typically safe; other strains require stronger antibiotics such as Bactrim. However, she adds, “the fear is that the MRSA strains will become even more resistant to the antibiotics we have, and the infections will become more serious and difficult to treat.” Luckily, over the years of dealing with MRSA, doctors have learned not to treat the problem with traditional antibiotics, which in the past allowed infections to worsen.
“MRSA is not more dangerous [than other forms of staph infections] in and of itself, but it is resistant to commonly used antibiotics, so it is more difficult to treat,” explains Glatt. “MRSA is not untreatable but, if left untreated or if improperly treated, it can progress.” Because MRSA symptoms look the same as those for Methicillin-Susceptible Staphylococcus Aureus (MSSA)—a strain of staph that can be treated with typical antibiotics—a physician must culture the bacteria to determine the strain. Although it is rare for a mild case in a healthy person to result in death, ignoring symptoms can lead to a fatal conclusion. Therefore, if you notice an abscess, a boil or a pus-filled lesion on a client’s skin, do not touch the area and tell her to have it checked out immediately by a physician.
A Nail Tech’s Prevention
Thankfully, you can take steps to make sure MRSA is not contracted at your salon. “In a nail salon, the following may spread MRSA infections: contaminated tools, working on clients who have an infection, or causing a break in the skin while working on a client,” says Kleinsmith. “Nail technicians must be very careful not to be too aggressive in cleaning under nails, pushing back cuticles or cutting the cuticles, which can lead to an opening in the skin.” Many nail pros have known for years that working gently and carefully will give the client a better service; in this case, it can actually impact her health.
Malo outlines some steps that you can take to prevent MRSA, all of which you should already do on a regular basis:
- Properly clean and disinfect all reusable areas and implements using an EPA-registered intermediate- to high-level disinfectant (remember the common areas as well, such as doorknobs, phones, desks, etc.); anything that touches one client’s skin should not touch another client’s skin until it has been cleaned and disinfected
- Throw out disposable items after each client
- Practice proper hand washing to help eliminate cross contamination; using soap and water, scrub for 20 seconds before and after each client, before and after eating, after handling money, etc.
- Use disposable, single-use towels in the bathroom
- Provide a barrier, such as a towel, between the client and communal surfaces (i.e., your nail table)
- Cover any pre-existing lesions or cuts on a client with a clean, dry dressing; use medical-grade gloves if you or the client has lesions on an area that may experience contact during the service
- Post cleaning and disinfecting protocols so all staff members are aware of the proper cleaning and disinfecting methods, and have an appropriate processing area to receive, clean, disinfect and sterilize items
- Salon owners must give technicians enough time to clean and disinfect between appointments. If the product states on the label that it requires 10 minutes to work fully, then the product takes 10 minutes to kill the pathogens—not five or eight minutes!
By following these guidelines, you will cut down on the risk of MRSA that everyone faces during skin-to-skin contact. This kind of protection is crucial for both your clients’ and your own well-being. Because—let’s face it—the biggest risk isn’t having your name in the news or having your license taken away; it’s knowing that you have endangered a client or, in the worst case scenario, created a serious health problem or caused a death. However, Glatt offers some grounding advice: “Techs don’t need to go crazy with worry about MRSA, but they definitely shouldn’t ignore it either; they need to be aware that diseases can be transmitted. In other words, take care of your clients, or they’ll become my patients.”
Tracy Morin is a freelance writer and editor based in Oxford, MS.











