Lack of moisture in hands and feet can result in any of these common problems. Here’s how to not hang your clients out to dry.
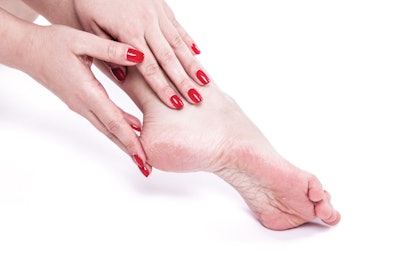 female legs with overdried dehydrated dry skin on heels closeup, cracked and dry skin on heels
female legs with overdried dehydrated dry skin on heels closeup, cracked and dry skin on heels
From blurring fine lines to fading unsightly brown spots, finding solutions to our collective skincare concerns has never been easier. Why, then, are so many nail salon clients still coming in with flaky, scaly, moisture-starved hands and feet? For starters, these extremities tend to come into contact with more elements and irritants than other parts of the body—and winter weather can be particularly punishing. Further, dry skin is often dismissed as a minor irritation rather than a serious issue. But, as a nail tech, you have a unique opportunity to address some of the most common conditions that may be plaguing your clients: chronically dry cuticles, cracked heels and eczema.
Caring for Cuticles
Most clients think of their cuticles as annoying “extra” bits of skin that they’d prefer were not there at all. In fact, they are likely confusing the cuticle with the eponychium—the strip of living skin that borders the base of the nail plate. The eponychium can be pushed back to expose and remove the cuticle (which is the scrim of non-living tissue adhered to the nail plate itself), but the cuticle is a small structure with an important function. “This scrim protects the area between the nail and epidermis, and the matrix (at the posterior of the nail) from bacterial invasion,” explains Janet McCormick, co-owner of Nailcare Academy in Fort Myers, Florida.
The eponychium only becomes pesky when it isn’t properly cared for and severe dryness results. The signs and symptoms of severely dry eponychia may include irritation, inflammation, itchiness, sensitivity, roughness, flaking and scaling, severe redness, and cracks than can bleed. Excessive exposure to cold or windy conditions and frequent contact with water (such as daily dish washing) or chemicals (such as cleaning solvents) are common causes, as is age. “Our body’s sebaceous glands slow their oil production as we age, causing our skin to dry out more easily,” McCormick notes. “So, an older person will have drier skin than a younger person who practices the same self-care.” Overall dehydration in the body, as well as chronic illnesses, such as diabetes, are other potential culprits.
RELATED: How to Fix Weak Splitting Nails
When working on a client with dry eponychia, first, do no harm. “Do not cut the skin except for the flagging, ‘trim me, trim me’ dry, dead areas,” McCormick warns. “Treat with moisturizing products designed for the area, and send a product home with the client for daily use.” This is an ideal retail opportunity; recommend products to your clients, such as nourishing cuticle oils packed with vitamins A and E, and hand and cuticle creams boasting naturally moisturizing hyaluronic acid. “Emphasize that the client must wear protective gloves when exposing hands to water or chemicals, outdoor gloves when exposed to cold and wind, and SPF in the sun,” McCormick adds.
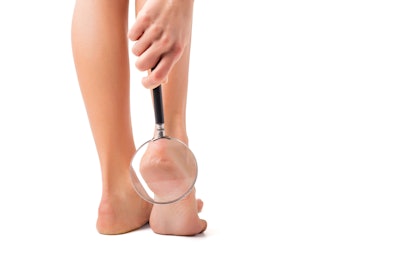 Woman with magnifying glass looking at heels
Woman with magnifying glass looking at heels
Helping Cracked Heels
Feet take a lot of abuse, notes Vicki Malo, president of the North American School of Podology in Toronto. “We lead high-stress, fast-paced lifestyles, and we don’t always eat or exercise right,” she notes. What does that have to do with dry feet? Everything. “Lack of self-care can lead to a breakdown of our circulatory system, which affects lower extremities first because they’re farthest from the heart,” Malo explains. “With this breakdown comes intercellular water loss, and that affects the skin: It gets microlesions and can’t hold in moisture.” Combine that with wearing open-heeled shoes or flip-flops, or going barefoot altogether, and the feet get even drier. Fail to address the issues, and damage and trauma follow. “The skin becomes compromised and that can lead to cracks, or fissures, in the heel,” Malo says. Although dry heels don’t always lead to cracks, “It’s rare to see a fissure without dry skin,” she adds.
In its early stages, the problem is easy to overlook. Perhaps the heels start to feel a little rough, maybe catch a little on the client’s socks—but a closer look reveals a budding problem. “You start to see these little dry lines, which are superficial cracks in the outer layers, or stratum corneum, of the skin, but the client isn’t aware of them,” Malo says. “However, they can get worse every time pressure is placed on the foot. Remember, we strike at our heels first; we bang down on them pretty hard. As a result, the skin can split open and create fissures that even reach the dermal layer.” Deep fissures can cause pain and bleeding. Even worse, they create a portal of entry for bacteria. “A bacterial infection could even turn into cellulitis,” warns Malo, though she notes that this risk is greater for people who are immunocompromised, such as those with diabetes and the elderly.
Nail techs should never work on pedicure clients who present with deep or bleeding heel cracks, but instead refer them to a medical professional. If the cracks are superficial, proceed with caution. “Make sure everything you do is hydrating,” Malo says. “Don’t soak the feet in anything caustic or dehydrating, like salts. Don’t file roughly around cracks, and when filing, go with the crack and never across or against it.”
Heel cracks are a preventable problem. “With monthly pedicures and home conditioning of the feet, cracking is not likely to happen,” McCormick says. Hydrating products abound for both prevention and maintenance, but make sure your recommendations contain naturally humectant ingredients, such as urea and spirulina, which will penetrate the stratum corneum. Advise clients to avoid walking around barefoot, choose sandals that hold heels in place and encourage circulation to the feet with targeted calf and foot exercises.
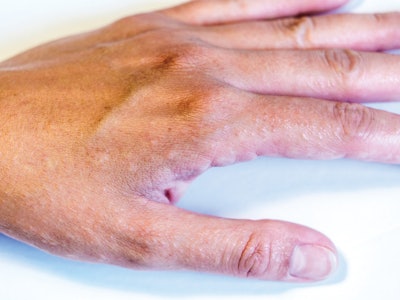 Closeup of hand with dyshidrotic eczema isolated on white background
Closeup of hand with dyshidrotic eczema isolated on white background
Easing Eczema
The common skin condition known as eczema is actually a group of conditions. The National Eczema Association (NEA) identifies eight types, including hand eczema and dyshidrotic eczema, which primarily affects the edges of the fingers, toes, palms and soles of the feet. Symptoms can range from mild to severe, and include dry, red, intensely itchy and sensitive skin, blisters and rough or scaly patches. Sometimes there’s oozing, crusting or swelling. Just as there are multiple types of eczema, there are multiple causes. Allergic reactions are a common culprit, usually related to topical exposure to the allergen. “Many people think that eczema is related to food, but after the age of 1 it’s much less likely that food has caused the problem,” notes Richard Caplan, MD, professor emeritus of dermatology at the University of Iowa College of Medicine in Iowa City. People who are genetically predisposed to eczema “tend to have dry skin, and the drier the skin, the more likely they are to scratch and aggravate the problem,” Dr. Caplan notes. Emotional stress is often a trigger, as well.
Most nail clients usually know if they have eczema and have probably already seen their doctor about it because it’s uncomfortable, says McCormick. “Usually, they keep it controlled with over-the-counter or prescription oral or topical medications,” she adds. Even so, you must mind the condition during nail services to avoid causing an outbreak. “Ask the client about her triggers, and know the ingredients in your products so you can avoid using anything that may pose a problem,” advises McCormick. “Moisturizing is important during the treatments, and any actively afflicted areas must be fully avoided.” Fortunately, the NEA has created a Seal of Acceptance to designate certain products they deem safe for people who suffer from eczema. To learn more, visit nationaleczema.org and click on the “Eczema Products” tab.
What’s your best advice on maintaining your clients’ skin moisturized during the winter? Let us know in the comments below!
-Linda Kossoff is a health and beauty writer based in Los Angeles.
[Images courtesy of Getty Images]
This article was first published in the December 2017 issue of NAILPRO
READ MORE:
Cracked Heels











