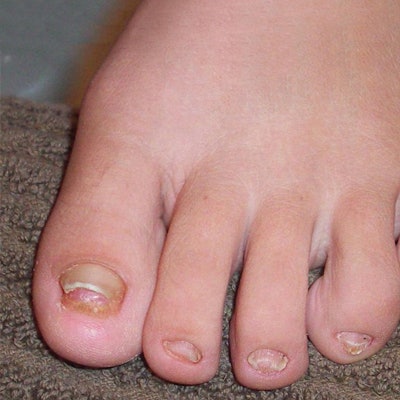
 Nail Atrophy Causes
Nail Atrophy Causes
Onychatrophy isn’t an exceedingly common condition, but it can get a bit confusing with the different terminology used to describe it. You may have heard of onychatrophia (this is a Latin-based word, according to Richard K. Scher, MD, adjunct professor of dermatology at the University of North Carolina in Chapel Hill) or onychatrophy (a word most commonly used in the medical community), but in layman’s terms, both describe atrophy of the nail—scarring that can be caused by a variety of factors. Regardless of its cause, nail techs need to be careful when faced with clients who exhibit this condition.
Common Causes of Nail Atrophy
Atrophy of the nail is defined by Merriam-Webster as “an atrophic or underdeveloped condition of the nails.” Scher explains that you can recognize nail atrophy because the nail plate will look a certain way: It might not grow at all, grow partially or show a partial loss of the nail. It’s a subset of nail dystrophy, a nonspecific word that simply describes an abnormal-looking nail. Scher, who has written five books on nails, relates some of the causes of nail atrophy.
Trauma Damage is by far the most common cause of atrophy of the nail. A client who hits her hand with a hammer or slams her finger in a car door often causes injury to the nail matrix, which is the growth center of the nail, according to Doug Schoon, chief scientific adviser for CND, in Dana Point, California. For instance, he notes that runners cause injury to their toes from wearing too-small running shoes; feet may swell up to a full size larger when running, and toenails (often on the big toe) can push up against the shoe, especially if the nail is too long. Scher adds that it depends on how severe the trauma was whether or not the scarring will be permanent and lead to atrophy. Minor injuries won’t cause enough damage to the nail matrix to lead to this problem. Generally, the nail simply falls off and grows back without further complication. However, you need to be aware that you can also cause trauma that leads to nail matrix damage if you push, trim or cut too aggressively in the cuticle area.
Lichen Planus: The National Center for Biotechnology Information (NCBI) describes lichen planus as a disease of unknown origin (but likely linked to an allergic or immune reaction) that causes an itchy rash on the skin or in the mouth. Skin lesions or shininess may also be present.
Connective Tissue Diseases: This group of diseases can include lupus (an autoimmune disorder), scleroderma (the NCBI notes that this can also cause the skin to tighten so that fingers lose mobility) or dermatomyositis (creating inflammation and a skin rash).
Bullous Diseases: These are also called blistering diseases. Mosby’s Medical Dictionary defines this group as “any of a number of conditions characterized by the formation of bullae [blisters larger than 1 centimeter wide] covering large portions of the skin surface.” This group includes Stevens Johnson Syndrome (a severe adverse reaction to medication), which can lead to permanent scarring if not treated early, Scher explains. Similarly, a severe burn that causes blistering can also lead to nail atrophy.
Heredity: Some people are simply born with atrophy of the nails for unknown reasons.
Scher notes that no matter the cause of the nail atrophy, the nail looks about the same—abnormally small—with symptomatic characteristics visible. Symptoms can include the nails to appear thin, discolored or rudimentary.
At the Station
Treating nail atrophy itself is impossible, but if a medical condition is causing it, seeking treatment for that condition is crucial and may help prevent further damage. If you notice a client with atrophy, don’t work on the nail, and ask if she knows the cause. Whether she says it’s due to trauma or thinks she knows the underlying cause, point her to a medical professional who can examine her. “The client wants to make sure there’s nothing else going on—for example, cancer of the nail bed creates scarring and could masquerade as nail atrophy,” says Scher. “If a nail tech sees any nail that looks abnormal, her obligation is simply to say, ‘See a dermatologist.’”
Schoon adds that a suspect nail is more susceptible to infection or fungus, so it’s crucial you don’t risk your livelihood by interacting with it. Even after a dermatologist has determined the cause, you’ll want to steer clear. “If it’s not a healthy nail, a nail tech is not licensed to work on it,” Schoon asserts. “A doctor can’t give permission to do something unsafe—even if the doctor says it’s OK, under what authority is he speaking?” In other words, because a doctor might not know exactly what products will be used in the salon, you should avoid working on the nail entirely.
If you notice a client with atrophy, don’t work on the nail, and ask if she knows the cause. If you see any nail that looks abnormal, your obligation is simply to say, “See a dermtologist.”
Unlike muscle atrophy, which simply describes a loss of tissue and can be remedied, nail atrophy relates to scarring—meaning permanent damage, just as a scar on skin would be permanent. If you see a client with this issue, make sure you proceed accordingly by sending her to a medical professional and avoiding contact. As a rule, erring on the side of caution will help you stay out of hot water when dealing with abnormal nails.
– Tracy Morin
Image: Courtesy of Danalynn Stockwood











